What does the pill do to your testosterone? Oral contraceptives, also known as birth control pills, are used by many women today to prevent pregnancy, stabilize unpredictable cycles, and even aid in the treatment of acne. When taken daily, women reduce the risk of becoming pregnant through three mechanisms:
- Ovulation suppression
- Thinning of the uterine lining
- Thickening of cervical mucus
The pill suppresses ovulation through the interference of normal estrogen and progesterone fluctuations that occur in women who are not pregnant.
The Hypothalamic-Pituitary-Ovarian Loop: FSH, LH, and GnRH Hormones
The hypothalamic-pituitary-ovarian loop is altered by exogenous, synthetic hormones present in birth control pills, and thus ovulation is suppressed.
This is achieved by keeping the amount of progesterone and estrogen consistent, which lower the amount of follicle-stimulating hormone (FSH) and luteinizing hormone (LH) secreted. FSH and LH are two hormones necessary for the maturation and ovulation of follicles (the structure containing the egg).
This whole mechanism is regulated by gonadotropin-releasing hormone (GnRH) secreted by neurons in the hypothalamus. Progestogen, the term for any synthetic progesterone, is responsible for thickening mucus in the cervix, making it more difficult for sperm to reach the egg, and thinning the uterine lining, which reduces the probability that an egg will successfully attach.
Synthetic versions of naturally occurring hormones, progesterone and estradiol, are designed to mimic the natural hormones produced by female reproductive organs—the ovaries. These pills can either contain one single hormone (a progestogen) or two hormones (a progestogen and estrogen).
Although the pill does not contain any form of testosterone, the synthetic estrogen and progesterone hormones may adversely affect testosterone in women.
Testosterone in Women
Testosterone in women is important for bone density, fat distribution, sexual desire and arousal, energy, and mood.
Interestingly enough, some of the most commonly reported side-effects of oral contraceptive use are decreased libido, weight fluctuations, and increased mood swings, all conditions influenced by testosterone.
If there is no form of testosterone in BCPs, why does this seem to correlate?
Sex Hormone-Binding Globulin (SHBG) Synthesis and Testosterone in Women
One possible culprit is sex hormone-binding globulin (SHBG).
This glycoprotein binds testosterone and estrogen to transport them throughout the blood. SHBG synthesis is stimulated by estrogens in the liver. Therefore, since estrogen is being added to the body by oral contraceptive pills, it increases the amount of SHBG being produced. When bound to SHBG, sex hormones are inactive and not biologically available. Thus, when there is more SHBG present, there is less free testosterone available for use.
The estrogenic component in virtually all oral contraceptives is thought to be 600 times more powerful in stimulating the synthesis of SHBG than natural estradiol, the most powerful form of natural estrogen (Mashchak et al., 1982).
Studies have found that the use of combined oral contraceptives increase SHBG levels tremendously as compared to those who have never used oral contraceptives, leaving women who take the pill with significantly lower amounts of free testosterone (Weigratz et al., 1995, Coenen et al., 1996, Wiegratz et al., 2003, Zimmerman et al., 2013). And remember, low testosterone may lead to low energy, undesirable weight changes, and decreased sexual desire.
It is important to note that synthetic hormones affect every individual differently. For some, these potential side effects are worth the benefits of using BCPs. Nonetheless, knowing how the pill works within your body may help you decide if beginning or continuing the use of oral contraception is right for you.
References:
Bowen, R. (13 May 2004). Gonadotropins: Luteinizing and Follicle Stimulating Hormones. Retrieved from http://arbl.cvmbs.colostate.edu/hbooks/pathphys/endocrine/hypopit/lhfsh.html
Coenen, C.M., Thomas, C.M., Borm, G.F., Hollanders, J.M., & Rolland, R. (1996). Changes in androgens during treatment with four low‐dose contraceptives. Contraception, 53, 171–176.
IPPF. (2013). Oral contraceptives (the pill). Retrieved from http://www.ippf.org/our-work/what-we-do/contraception/oral-contraceptives-pill
Mashchak, C.A., Lobo, R.A., Dozono‐Takano, R., Eggena, P., Nakamura, R.M., Brenner, P.F., & Mishell, D.R. (1982). Comparison of pharmacodynamic properties of various estrogen formulations. Am J Obstet Gynecol, 144, 511–518.
USC Fertility. (2016). Learn Fertility Basics: Human Reproduction Hinges on Female Ovulation. Retrieved from http://uscfertility.org/fertility-treatments/fertility-basics/
Wiegratz, I., Jung‐Hoffmann, C., & Kuhl, H. (1995). Effect of two oral contraceptives containing ethinylestradiol and gestodene or norgestimate upon androgen parameters and serum binding proteins. Contraception, 51, 341–346.
Wiegratz, I., Kutschera, E., Lee, J.H., Moore, C., Mellinger, U., Winkler, U.H., & Kuhl, H. (2003). Effect of four different oral contraceptives on various sex hormones and serum‐binding globulins. Contraception, 67, 25–32.
Zimmerman, Y., Eijkemans, MJC, Coelingh Bennink, HJT, Blankenstein, MA, & Fauser, BCJM. (2013). The effect of combined oral contraception on testosterone levels in healthy women: a systematic review and meta-analysis. Hum. Reprod. Update, 20(1), 76-105.
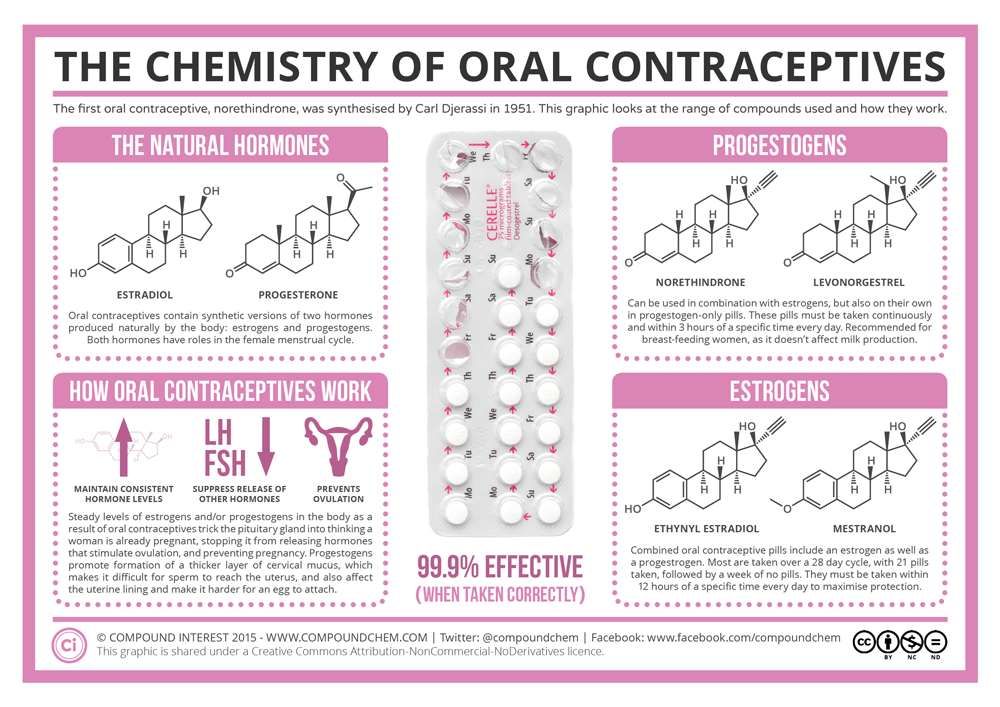
The Chemistry of Oral Contraceptives [Digital image]. (2015, February 3). Retrieved March 13, 2015, from http://www.compoundchem.com/2015/02/03/oral-contraceptives/

