A poster recently presented at the American Society for Nutrition provides evidence that the NeuroWellness Program™ for neuroendocrine health supports weight management when combined with clinician care. Researchers found significant improvements in body mass index (BMI), weight-related quality-of-life concerns (comorbidities), and biomarkers important to weight management.
An individual’s weight plays a significant role in that person’s health and quality of life. We report here correlations between weight and mood, cognitive function, sleep, and cardiovascular function to name just a few. Underlying imbalances in the neuroendocrine system, specifically the hypothalamic-pituitary-adrenal and thyroid (HPA-T) axis, may explain the wide variety of comorbidities associated with unhealthy weight. The results of this study indicate imbalances in the HPA-T axis are likely contributors to some of the difficulties in a patient’s weight management.
The Study
This study evaluates the impact of the NeuroWellness Program and clinician care on BMI and various self-reported quality-of-life markers along with neuroendocrine markers.
The NeuroWellness Program consists sequentially of neuroendocrine testing, personalized neuroendocrine analysis reporting, and Targeted Nutritional Therapy™ (TNT). This is a cycle. Individuals typically report optimal results after completing three cycles of the NeuroWellness Program.
Two cohorts were examined, one consisting of 703 patients and another subgroup of 279 patients with BMI >29. All individuals went through three cycles of the NeuroWellness Program, used Sanesco’s TNT formulas, and were pharmaceutically naïve. It is noteworthy that these individuals were not seeking care for weight management.
Results for both cohorts were determined by comparing baseline data with the data obtained after the third cycle of testing and statistically significant improvements were found in three areas related to weight.
Benefits of the NeuroWellness Program and Clinician Care on Weight Management
BMI
According to the Centers for Disease Control (CDC), BMI groups people into categories based on weight divided by the square of the height using the metric system. Though not diagnostic of body fat or individual health, it is used as a screen for identifying weight categories that may be associated with certain health problems. BMIs from 19-24 are considered “healthy” whereas other BMIs may be associated with significant health concerns.

The study found statistically significant improvements in BMI for the main cohort and the sub-group after three cycles of the NeuroWellness Program including use of Sanesco’s TNT formulas. However, the percent change was greatest and most significant for the BMI >29 cohort (see table for details). The change in BMI distribution (see graphs) shows how significantly the mean and median BMIs changed for cohort 2.
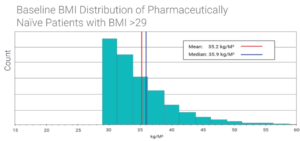
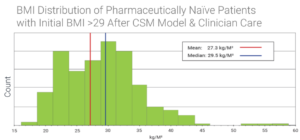
Comorbidities Related to Weight
At the time of each test, patients completed a quality-of-life assessment where they rated how much various aspects of health were affecting their quality of life on a scale of 0-4, with 4 indicating the most impact.
For this analysis, 23 quality-of-life aspects that research indicates either impact or are impacted by weight were assessed. Aspects range from mood to sleep to cravings, and even cognitive function. Of the 23 weight-related, quality-of-life aspects examined, 16 improved significantly (p <0.05 or better) for the overall cohort.
For individuals with BMI >29, statistically significant improvements were found for 22 of the 23 quality-of-life indicators.
Both cohorts experienced statistically significant improvements (p<0.005) in poor stamina and dark thoughts. For those looking to manage weight, endurance and a positive attitude are essential. Some additional quality-of-life issues might impair the ability to manage weight by interfering with the ability to exercise, to stick to dietary guidelines, and for the body to heal.
Individuals with BMI >29 reported statistically significant reduction in aches and discomfort (p<0.005), which may be a factor discouraging these patients from exercising. This cohort also report significantly less desire for sugar, salt, and alcohol (p<0.05). Fewer cravings make it easier to stick to nutritional guidelines, and a good night’s sleep (p<0.05) allows the body to repair itself.
Neuroendocrine Markers Important for Weight Management
In research, there are still questions about fundamental aspects of how the HPA-T axis impacts weight management. One recent meta-analysis did not find a correlation between cortisol and weight (Tenk et al, 2018) though exercise lowers stress by decreasing cortisol. However, a resulting hypothesis from this weight poster is, “HPA-T axis dysregulation of glucocorticoids, lack of adrenal tone, and disruption of neuroactive metabolites may be at the heart of weight-related comorbidities.”
Indeed, the analysis of the data presented in this poster indicate statistically significant improvements in neurotransmitters and hormones playing key roles in weight management and related concerns. This finding provides evidence that addressing balance within the neuroendocrine system is essential for weight management.
The BMI >29 cohort experienced significant changes in:
- Serotonin (p<0.005)
- Norepinephrine (p<0.005)
- Epinephrine (p<0.05)
- Glutamate (p<0.005)
- Morning cortisol (p<0.005)
- Evening cortisol (p<0.05)
The NeuroWellness Program and Clinician Care- Proven Support for Weight Management
Whether you want to give your weight management program a boost or are simply seeking to improve multiple quality-of-life indicators, the NeuroWellness Program is a proven approach.
Find or become a Sanesco provider to add the NeuroWellness Program approach to your weight management regimen now or contact us to learn more.
References
- Watkins R and Schmitt J. Obesogenic Alterations in Adrenal Function and Neurotransmitter Balance Improved with Dietary Supplementation. American Society for Nutrition Poster Presentation. 2019.
- Centers for Disease Control and Prevention. Healthy Weight. 2015 May 15. Accessed: January 15, 2020. At https://www.cdc.gov/healthyweight/assessing/bmi/index.html
- Tenk J, et al. PLos One. 2016;11(11):e0166842.
Disclaimer: Sanesco in its relationship to its clinician customers imposes no oversight on how the NeuroWellness Program is employed. Conversely, Sanesco does not take into account the advice clinicians may have given patients with regard to diet, exercise or dietary supplementation.


